01 July, 2015
The number of multi-drug-resistant tuberculosis cases is rising. Multi-drug-resistant TB results from a bacterium – a group of small living things that can cause disease. The bacterium is hard to kill because it has become resistant to two or more common antibiotics.
But researchers have reported some good news: the multi-drug-resistant form of TB is less infectious than other forms of the disease among a patient's close friends and family members.
In 2013, the World Health Organization reported almost 500,000 cases of multi-drug-resistant TB. Anti-microbial tuberculosis often infects patients who were treated earlier for TB or those infected with HIV, the virus that causes AIDS.
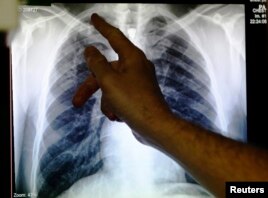
A doctor points to an x-ray showing a pair of lungs infected with TB (tuberculosis) in Ladbroke Grove in London, England, Jan. 27, 2014.
Often, these patients did not complete the drug treatment ordered by doctors, giving the bacterium time to develop defenses against the antibiotics.
Experts say treatment for multi-drug-resistant TB can take up to two years and require as many as six strong, less modern antibiotics. These antibiotics often have a higher death rate than today's antibiotics because of the drugs' toxicity – the harm they can cause to the body.
But British and Peruvian researchers are offering some hope. Their findings were published in the journal PLOS Medicine.
The researchers found that drug-resistant forms of TB have a lower "fitness" for spreading to people close to those infected with it. That means the disease does not spread as aggressively as non-drug-resistant TB.
Louis Grandjean works at Imperial College London. He led the study in Peru.
"In becoming drug-resistant, the bacteria undergo what it called a ‘fitness' cost. So it's able to survive in the environment of antibiotics, but it's less able to jump from person to person and cause disease."
For three years, the researchers followed more than 1,000 family members and friends of people with multi-drug-resistant tuberculosis. They also followed more than 2,300 contacts of patients with non-drug-resistant TB in Lima.
Thirty-five of the multi-drug-resistant contacts became sick during the study. Of those in contact with patients with non-drug-resistant TB, 114 of them became sick.
The researchers found that contacts of the multi-drug-resistant group were 44 percent less likely than the others to get sick with tuberculosis.
Yet Louis Grandjean says that does not make multi-drug-resistant TB any less of a threat.
"It's still a huge problem, despite what we found in the study, which is encouraging and suggests that the tuberculosis program, which is working at full capacity to try to control multi-drug-resistant tuberculosis, is still a great problem."
Given the seriousness of the threat, he says, the world cannot ease up on treatment efforts and guarding against the disease.
I'm Jim Tedder.
VOA's Jessica Berman reported on this story. George Grow adapted it for Learning English. Ashley Thompson was the editor.
______________________________________________________________
Words in This Story
antibiotics – n. drugs used to kill harmful bacteria
anti-microbial – adj. destroying or limiting the growth of very small organisms
fitness – n. the ability of an organism to survive
undergo – v. to experience